Psoriasis is a common auto-immune condition that leads to unsightly and often painful patches of excess skin cells to appear all over the body, but particularly on the joints. These can cause a great deal of irritation and have a tendency to worsen in response to certain triggers, including stress.
Other than the fact that it is caused by an overactive immune system, the cause of the disease has been very poorly understood until recently. New advances in stem cell technologies have led to a better understanding of what causes the disease and have presented new possible forms of treatment for it as well.
While the exact nature of the condition is still largely unknown, vast strides are being made towards pinning down an exact cause for the disease and using this information to develop a new kind of treatment for the condition.
What is Psoriasis?
Psoriasis is a very common skin condition caused by the body’s own immune system. It causes thick, irritating patches of excess skin cells to form on the surface of the skin. These patches of excess skin cells are known as plaques, and usually appear red and scaly.
These plaques are usually dry and can cause itching or irritation in those who suffer from the condition. These plaques commonly appear on the elbows and knees but can also appear on other areas of the body such as the palms of the hands or soles of the feet.
Currently the condition has no permanent cure, when someone suffers from the disease, they will remain a sufferer throughout their life. Even though they might not continually suffer from these plaques, those who experience the condition will experience flare-ups intermittently from a variety of causes. These triggers for psoriasis include:
- Stress
- Infections or other illness
- Injury to the skin
- Some medications
- Weather and environmental conditions, particularly cold weather
It is important to try to identify the triggers that an individual experiences to try to reduce the number of flare-ups the patient experiences to help better manage the condition.
Psoriasis Causes
The main underlying cause of psoriasis is still unknown. However, there is some information available about how the plaques form and what causes their formation.
It is well-understood that there is a significant genetic component to contracting the disease. There are a wide variety of different genes that can put an individual at risk of developing psoriasis, but none of them are a guaranteed cause. Instead, the genes make it more likely that an individual will develop the disease, with the exact mechanism that determines whether an individual does indeed become a sufferer still being unknown.
Whatever the cause, in those who suffer from psoriasis, the body’s T-cells are affected and act differently to those found in a healthy individual.
The T-cells are part of the body’s immune system that help to combat infections. In patients who suffer from psoriasis, these T-cells mis-identify the patient’s own skin cells as foreign objects. This causes them to attack the skin cells, which leads to the formation of the scaly plaques.
When the T cells attack the skin, blood vessels in the skin enlarge and the immune response leads to an above-average rate of production of new cells. This leads to an overproduction of skin cells, and an overproduction of cells from the immune system as well. The immune response continues to build up and produce more and more skin cells which develop into the characteristic scaly patches.
Malfunctioning Stem Cells May Be the Underlying Cause
Recent advances in our understanding of stem cells have led to a possible identification of the cause of psoriasis that would allow researchers to develop new treatments that directly address this cause.
Research from the Brigham and Women’s Hospital identified a change in the epigenetic component of DNA in the stem cells found in the skin that is present only in psoriasis patients and not in patients suffering from other types of skin disease.
Epigenetic factors work hand in hand with genetic factors to determine how various genes within the body get expressed. While the DNA contains the instructions to create various different proteins, epigenetics describes the kind of structural modifications made to the outside of the DNA molecule that determines which of the genes are processed and which of these instructions get read. These epigenetic factors explain why some genes are expressed in some cells to produce proteins specific to that cell, and not others.
The change found by researchers from the Brigham and Women’s hospital is suspected to be a direct cause of psoriasis in at least some patients, and so finding ways to revert this change could lead to a cure for the condition.
A number of other researchers have also found changes in the DNA and epigenetic codes of the stem cells that produce the majority of cells found within the skin that are linked to psoriasis. At the moment it’s not entirely clear which of these contributes most to psoriasis, or if there is a single key change that could be targeted for treatment.
Epigenetic abnormalities have also been detected in other kinds of stem cells found throughout the body, including the hematopoietic stem cells that differentiate into the blood cells used within the body. Research into how these changes interlink and which are the most important is ongoing and will hopefully lead to new avenues of treatment for psoriasis.
Treatment Options
Though there are as yet no permanent cures for psoriasis, there are a number of possible treatments that provide some level of relief. The goal of treating psoriasis currently is to reduce the impact of the symptoms while also minimizing the number of flare-ups experienced by the patient.
Topical Treatments
There are a variety of skin creams that can be applied to the psoriasis plaques to reduce the amount of itching or flaking of these plaques. There are also a number of creams that can be applied regularly to the skin to reduce the chance of plaques appearing, or to reduce the severity of those that do form.
Phototherapy
One possible treatment method involves exposing the skin to artificial light to reduce the rate of growth of the excess skin cells. Ultraviolet light is used in quantities and for periods of time dependent on the patient to ensure an adequate amount of exposure for their particular condition.
Medications
There are a variety of medications currently available that reduce the action of the immune system and can be used to treat a wide variety of auto-immune disorders. They are especially likely to be prescribed in cases where the outbreaks affect a wide range of the body, rather than just a particular area. Vitamin A can also be used for treatment in this case.
Stem Cell Therapy for Psoriasis
Given that stem cells play a key role in the proliferation of the cells that are involved with flare-ups of psoriasis, scientists have begun to develop treatments for psoriasis that make use of stem cells to treat the condition. By targeting the defective stem cells that produce the cells that lead to plaque formation, it is hoped that healthy cells can be produced in patients who suffer from psoriasis so that the plaques won’t form, effectively providing a cure.
Further investigation into the relationship between stem cells and psoriasis have identified that stem cell populations in a variety of locations throughout the body have similar epigenetic variations to those found in the stem cells in the skin. It is therefore thought that psoriasis is a more complicated condition than had been previously imagined and affects more of the body than just the skin.
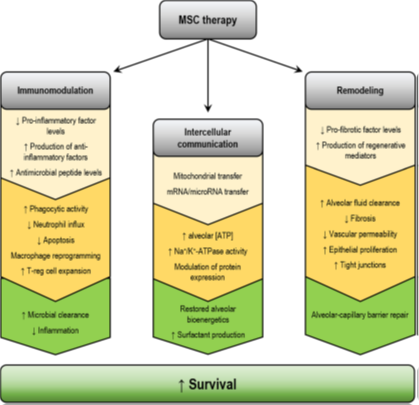
This kind of treatment is known to be safe and relatively non-invasive and has been used in a wide variety of other situations to treat other diseases. When stem cells are transplanted to an individual, they produce a wide variety of growth factors and other chemicals that promote the growth and repair of damaged cells, while also repressing the immune response. These interactions have been shown to treat a wide variety of different autoimmune conditions and it is hoped that they will be able to treat psoriasis as well.
Evidence of the Effectiveness of the Treatment
Currently there has not been significant research into using stem cells to treat psoriasis. Although the treatment looks promising, the new information about the role that stem cells play in causing psoriasis has not been sufficiently well explored to come up with a comprehensive treatment program for the condition using stem cells.
That said, there have been a number of studies that have looked at particular cases in which stem cell transplants have been used as a treatment for those suffering from psoriasis.
One such study published early in 2020 looked at how a treatment based on transplanting stem cells could help to treat psoriasis in a 19-year-old man. While it is not a full clinical study, it is a particular case study that contains valuable information.
In this instance, the patient received stem cell treatments by extracting stem cells from the gum tissue of a healthy individual that were then injected into the patient’s blood stream. The injection was repeated two more times at weekly intervals, and then after a pause of five weeks, three more injections were given at weekly intervals.
During this period, the plaques gradually disappeared, until a week after the final injection where the legions had disappeared completely. The patient was then followed up with three years after the initial treatment and was found to be free of psoriasis still.
This possible route of using stem cell injections that have been shown to be safe and non-invasive looks like an extremely promising possibility for future treatments. As more and more is understood about the role that stem cells play in causing this disease, hopefully a treatment that makes use of this understanding will be quickly developed.
Reach out to BioXcellerator today to learn more about how our team can help treat your psoriasis. We will develop a comprehensive treatment plan that will be unique to your needs.